The apoC3 inhibitor, Tryngolza (olezarsen), has been approved by the US Food and Drug Administration (FDA) for use in adults with familial chylomicronaemia syndrome (FCS) as an adjunct to diet.
Remnant cholesterol linked to ASCVD events in diabetes and impaired renal function
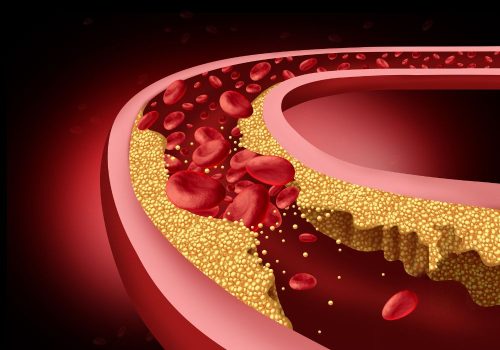
One in five atherosclerotic cardiovascular disease (ASCVD) events in people with diabetes can be attributed to elevated remnant cholesterol, according to an analysis of 3,806 individuals with diabetes identified among 107,243 people from the Copenhagen General Population Study (CGPS).1 Elevated remnant cholesterol was defined as levels higher than those in individuals with non-HDL-C <2.6 mmol/L (100 mg/dL), […]
Comparing FCS with MCS
Targeted DNA sequencing in 193 patients with severe hypertriglyceridemia has shone new light on differences and similarities between familial chylomicronaemia syndrome (FCS) and multifactorial chylomicronaemia syndrome (MCS). The study showed that patients with FCS were significantly younger than those with MCS (31.4±16.7 vs. 51.0±11.3 years; p=0.003), with earlier age at symptom onset (15.0±15.8 vs. 37.8±8.8 […]
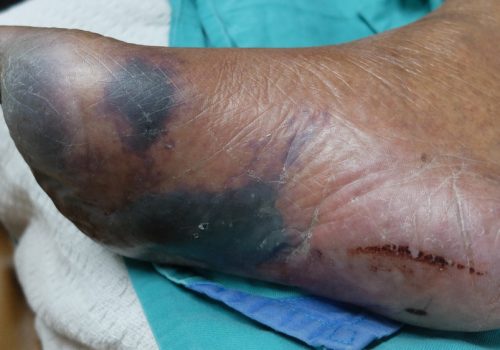
Pemafibrate shows potential for diabetic foot and gangrene
Encouraging results from an exploratory analysis of data from the PROMINENT trial showing that the potent and selective PPARα modulator, pemafibrate, reduced diabetic lower extremity ulceration and gangrene by 37% have been published in the Journal of the American College of Cardiology.1
Akiro Endo, discoverer of statins, remembered
Dr Jonathan Tobert, University of Oxford, UK, recalls the landmark statin research by Dr Akira Endo that has saved countless lives. Akira Endo, the Japanese scientist universally recognised as the discoverer of statins, died on June 5 at the age of 90. The medical importance of his discovery is arguably comparable with Fleming’s discovery of […]
Plozasiran topline results show promise in familial chylomicronaemia syndrome
Topline data from the Phase 3 PALISADE study (NCT05089084) in patients with familial chylomicronaemia syndrome (FCS) have shown that the apolipoprotein C3 (APOC3) inhibitor, plozasiran, significantly reduced median TG levels by up to -80% at month 10, with mean reductions in APOC3 of up to -94%.